Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (35): 6306-6313.doi: 10.3969/j.issn.2095-4344.2013.35.014
Previous Articles Next Articles
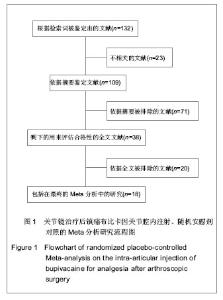
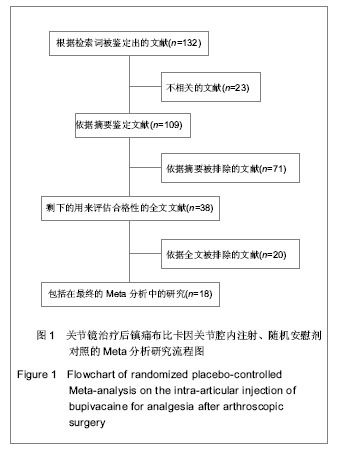
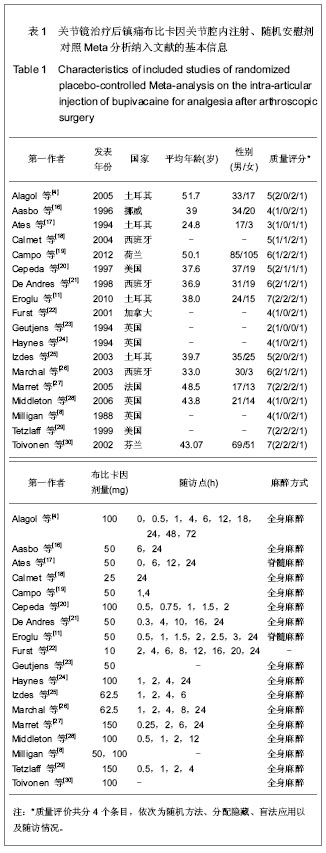
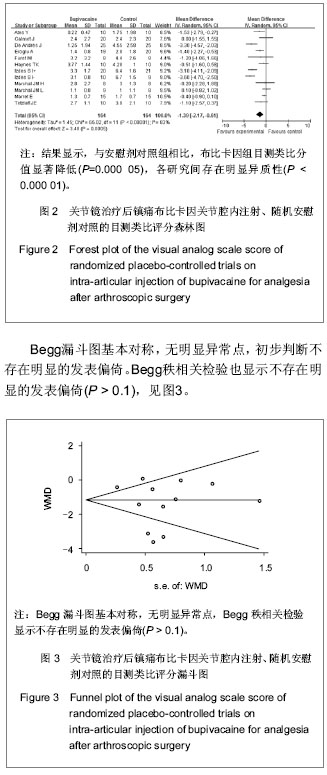
Analgesia after arthroscopic surgery: Randomly controlled Meta-analysis on intra-articular injection of bupivacaine placebo
Yang Tuo, Gao Shu-guang, Luo Wei, Li Yu-sheng, Xiong Yi-lin, Sun Jin-peng, Lei guang-hua
- Department of Orthopedics, Xiangya Hospital, Central South University, Changsha 410008, Hunan Province, China
-
Received:2013-05-24Revised:2013-06-08Online:2013-08-27Published:2013-08-27 -
Contact:Lei Guang-hua, M.D., Professor, Chief physician, Doctoral supervisor, Department of Orthopedics, Xiangya Hospital, Central South University, Changsha 410008, Hunan Province, China lgh9640@sina.cn -
About author:Yang Tuo★, Studying for master’s degree, Department of Orthopedics, Xiangya Hospital ,Central South University, Changsha 410008, Hunan Province, China 693673464@qq.com
CLC Number:
Cite this article
Yang Tuo, Gao Shu-guang, Luo Wei, Li Yu-sheng, Xiong Yi-lin, Sun Jin-peng, Lei guang-hua. Analgesia after arthroscopic surgery: Randomly controlled Meta-analysis on intra-articular injection of bupivacaine placebo[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(35): 6306-6313.
share this article
| [1] Pavlin DJ, Chen C, Penaloza DA, et al. A survey of pain and other symptoms that affect the recovery process after discharge from an ambulatory surgery unit. J Clin Anesth. 2004;16(3):200–206.[2] St-Pierre DM. Rehabilitation following arthroscopic meniscectomy. Sports Med. 1995;20(5):338-347.[3] Solheim N, Rosseland LA, Stubhaug A .Intra-articular morphine 5 mg after knee arthroscopy does not produce significant pain relief when administered to patients with moderate to severe pain via an intra-articular catheter. Reg Anesth Pain Med. 2006; 31(6):506-513.[4] Alagol A, Calpur OU, Usar PS, et al. Intraarticular analgesia after arthroscopic knee surgery: comparison of neostigmine, clonidine, tenoxicam, morphine and bupivacaine. Knee Surg Sports Traumatol Arthrosc. 2005;13:658-663.[5] 李学婷.膝关节镜术后2种镇痛方法比较[J].郑州大学学报:医学版,2007,42(5):999-1000.[6] 战民庆,牟宇科,尉建杰,等.膝关节镜术后注入关节腔小剂量吗啡复合布比卡因镇痛的临床应用[J].中国医师杂志,2009,11(2): 257-258.[7] Henderson RC, Campion ER, DeMasi RA, et al.Postarthroscopy analgesia with bupivacaine. A prospective, randomized, blinded evaluation. Am J Sports Med.1990;18:614-617.[8] Milligan KA, Mowbray MJ, Mulrooney L, et al.Intra-articular bupivacaine for pain relief after arthroscopic surgery of the knee joint in daycase patients. Anaesthesia. 1988;43: 563-564.[9] Chirwa SS, MacLeod BA, Day B.Intraarticular bupivacaine (Marcaine) after arthroscopic meniscectomy: a randomized double-blind controlled study. Arthroscopy. 1989;5:33-35.[10] Smith I, Van Hemelrijck J, White PF, et al. Effects of local anesthesia on recovery after outpatient arthroscopy. Anesth Analg.1991;73:536-539.[11] Eroglu A, Saracoglu S, Erturk E, et al.A comparison of intraarticular morphine and bupivacaine for pain control and outpatient status after an arthroscopic knee surgery under a low dose of spinal anaesthesia. Knee Surg Sports Traumatol Arthrosc.2010; 18:1487-1495.[12] Craft DV, Good RP.Delayed hypersensitivity reaction of the knee after injection of arthroscopy portals with bupivacaine (marcaine). Arthroscopy.1994; 10:305-308.[13] Goodwin RC, Parker RD.Comparison of the analgesic effects of intra-articular injections adminstered preoperatively and postoperatively in knee arthroscopy.J Knee Surg.2005;18:17-24.[14] Liberati A, Altman DG, Tetzlaff J, et al.The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol.2009;62:e1-e34.[15] Begg B, Mazumdar M.Operating characteristics of a rank correlation test for publication bias. Biometrics.1994;50: 1088-1101.[16] Aasbo V, Raeder JC, Grogaard B, et al.No additional analgesic effect of intra-articular morphine or bupivacaine compared with placebo after elective knee arthroscopy. Acta Anaesthesiol Scand.1996;40:585-588.[17] Ates Y, Kinik H, Binnet MS, et al.Comparison of prilocaine and bupivacaine for post-arthroscopy analgesia: a placebo-controlled double-blind trial. Arthroscopy.1994; 10: 108-109.[18] Calmet J, Esteve C, Boada S, et al.Analgesic effect of intra-articular ketorolac in knee arthroscopy: comparison of morphine and bupivacaine. Knee Surg Sports Traumatol Arthrosc.2004;12:552-555.[19] Campo MM, Kerkhoffs GM, Sierevelt IN, et al.A randomised controlled trial for the effectiveness of intra-articular Ropivacaine and Bupivacaine on pain after knee arthroscopy: the DUPRA (DUtch Pain Relief after Arthroscopy)-trial. Knee Surg Sports Traumatol Arthrosc.2012;20:239-244.[20] Cepeda MS, Uribe C, Betancourt J, et al.Pain relief after knee arthroscopy: intra-articular morphine, intra-articular bupivacaine, or subcutaneous morphine? Reg Anesth.1997;22:233-238.[21] De Andres J, Valia JC, Barrera L, et al.Intra-articular analgesia after arthroscopic knee surgery: comparison of three different regimens. Eur J Anaesthesiol.1998;15:10-15.[22] Furst IM, Kryshtalskyj B, Weinberg S.The use of intra-articular opioids and bupivacaine for analgesia following temporomandibular joint arthroscopy: a prospective, randomized trial. J Oral Maxillofac Surg.2001;59:979-983, 983-984.[23] Geutjens G, Hambidge JE.Analgesic effects of intraarticular bupivacaine after day-case arthroscopy. Arthroscopy.1994;10: 299-300.[24] Haynes TK, Appadurai IR, Power I, et al.Intra-articular morphine and bupivacaine analgesia after arthroscopic knee surgery. Anaesthesia.1994;49:54-56.[25] Izdes S, Orhun S, Turanli S, et al.The effects of preoperative inflammation on the analgesic efficacy of intraarticular piroxicam for outpatient knee arthroscopy. Anesth Analg. 2003; 97:1016-1019.[26] Marchal JM, Delgado-Martinez AD, Poncela M, et al.Does the type of arthroscopic surgery modify the analgesic effect of intraarticular morphine and bupivacaine? A preliminary study. Clin J Pain.2003;19:240-246.[27] Marret E, Gentili M, Bonnet MP, et al.Intra-articular ropivacaine 0.75% and bupivacaine 0.50% for analgesia after arthroscopic knee surgery: a randomized prospective study. Arthroscopy. 2005;21:313-316.[28] Middleton F, Coakes J, Umarji S, et al.The efficacy of intra-articular bupivacaine for relief of pain following arthroscopy of the ankle. J Bone Joint Surg Br.2006;88: 1603-1605. [29] Tetzlaff JE, Dilger JA, Abate J, et al.Preoperative intra-articular morphine and bupivacaine for pain control after outpatient arthroscopic anterior cruciate ligament reconstruction. Reg Anesth Pain Med.1999;24:220-224.[30] Toivonen J, Pitko VM, Rosenberg PH.Comparison between intra-articular bupivacaine with epinephrine and epinephrine alone on short-term and long-term pain after knee arthroscopic surgery under general anesthesia in day-surgery patients. Acta Anaesthesiol Scand.2002;46:435-440.[31] Møiniche S, Mikkelsen S, Wetterslev J, et al.A systematic review of intra-articular local anesthesia for postoperative pain relief after arthroscopic knee surgery. Reg Anesth Pain Med.1999;24:430-437.[32] 袁红斌,叶军青,王新华,等.小剂量吗啡关节内注射用于膝关节镜术后镇痛的临床观察[J].中国疼痛医学杂志,2000,6(4): 203-205.[33] 袁红斌,王成才,傅强,等.小剂量吗啡关节内注射用于膝关节镜术后镇痛的临床观察及机制探究[J].临床麻醉学杂志,2003,19(11): 667-669.[34] 吴宇黎,吴海山,李晓华,等.小剂量吗啡和倍他米松在膝关节镜术后镇痛中的应用[J].中国组织工程研究与临床康复,2007,11(39): 8018-8020.[35] Ruwe PA, Klein I, Shields CL.The effect of intraarticular injection of morphine and bupivacaine on postarthroscopic pain control. Am J Sports Med.1995;23:59-64.[36] Reuben SS, Sklar J.Pain management in patients who undergo outpatient arthroscopic surgery of the knee. J Bone Joint Surg Am.2000;82:1754-1766.[37] 李军,崔德荣.关节腔内注射氯诺昔康复合布比卡因、吗啡或丁丙诺啡用于膝关节镜术后镇痛的效应[J].蚌埠医学院学报,2008, 33(3):303-306.[38] 周向宏,宋杰.关节腔内注入吗啡和布比卡因用于膝关节镜术后镇痛[J].南通医学院学报,2003,23(3):317-318.[39] Karamanlio?lu B, Alagöl A, Turan FN.Preemptive oral rofecoxib plus postoperative intraarticular bupivacaine for pain relief after arthroscopic knee surgery. Agri. 2005;17: 29-33.[40] Koltka K, Koknel-Talu G, Asik M, et al.Comparison of efficacy of intraarticular application of magnesium, levobupivacaine and lornoxicam with placebo in arthroscopic surgery. Knee Surg Sports Traumatol Arthrosc.2011;19:1884-1889.[41] 潘昊,彭永海,王俊文,等.关节镜术后使用布比卡因加复方倍他米松镇痛的疗效观察[J].中国医院药学杂志,2008,28(19): 1701-1702. |
| [1] | Lu Yanqin, Yi Fang, Ju Wei, Li Wenjie, Lei Lei. Reparation of femoral defects with a Ca-P coated magnesium alloy scaffold carrying sustained release microspheres [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(2): 232-238. |
| [2] | Wang Xiao-ming, Duan Hao, Xia Bin, Wei Jian-min. Feasibility of lateral-position pedicle screw placement via combined anterior-posterior approaches in spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(39): 6333-6338. |
| [3] | Liu Yan-cheng, Xia Qun, Hu Yong-cheng, Zhang Ji-dong, Bai Jian-qiang, Ji Ning, Zhang Kuan. Evaluation of gait characteristics of cervical spondylotic myelopathy patients by a portable gait analyzer [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(11): 1774-1779. |
| [4] | Zhang Meng-yuan, Chen Ke-yi, La Xiao-lin, Deekshya Shrestha. A meta-analysis of clinical efficacy of fresh embryo transfer versus frozen embryo transfer in in vitro fertilization cycles [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(53): 9245-9250. |
| [5] | Yu Jie, Wang Yu-jie, Liu Yu, Ma Qi, Zhang Li-dong. Meta analysis of 2-μm laser in the treatment of non-muscle-invasive bladder tumor [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(53): 9251-9260. |
| [6] | Wang Lu, Jian Jie, Lu Hui-fang. Efficiency of resin infiltration versus fluride varnish for treatment of post-orthodontic white spot lesions [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(29): 5303-5308. |
| [7] | Ding Ming-xiang, Lin Shao-hua, Li Liang-ming, Hou Bo, Liang Chao-feng, Gong Jin, . Biocompatibility of an acellular brain tissue scaffold with bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(14): 2495-2500. |
| [8] | Zhou Yan, Piao Jin-hua, Jin Lian-hua, Yang Si-rui. null [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(1): 112-117. |
| [9] | Liu Ji-chun, Hu Hong-tao, Xu Guo-hua, Jiang Yu-quan, Xu Ning, Ye Xiao-jian. A modified method of isolating and culturing human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2012, 16(45): 8394-8397. |
| [10] | Chen Yun-fei1, Wang Yi2, Yang Hong-ji3. null [J]. Chinese Journal of Tissue Engineering Research, 2012, 16(5): 899-·902. |
| [11] | Wang Cheng-wei1, Li Hong-lin1, Zhao Bo1, Li Lu-bing1, Pa Er Ha Ti1, Wang Xue1, Zheng Hui1, A Man1, Yu Jian-hua2. Evaluation of meniscus injury by magnetic resonance imaging: A documentary analysis based on Science Citation Index from 2001 to 2010 [J]. Chinese Journal of Tissue Engineering Research, 2012, 16(4): 571-580. |
| [12] | Bai Chuan-yi1, Ning Ning1, Ling Wei2, Tian Zhen-xing2, Dang Xiao-qian1, Wang Kun-zheng1. null [J]. Chinese Journal of Tissue Engineering Research, 2012, 16(4): 585-588. |
| [13] | Zhou Zhong-xiao, Wei Xi-lin, Yao Jian-ru, Zhang Jian, Bian Gang, Li Jin-hui. Evaluation of biological hemostatic dressings and gauzes in surgical wounds [J]. Chinese Journal of Tissue Engineering Research, 2010, 14(51): 9635-9638. |
| [14] | Zhang Kun, Jiang Yi, Lü Li-zhi, Zhang Xiao-jin, Yang Fang, Chen Yong-biao, Cai Qiu-cheng, Pan Fan. Orthotopic liver transplantation for primary hepatic cancer [J]. Chinese Journal of Tissue Engineering Research, 2010, 14(44): 8357-8360. |
| [15] | Tian Bao-xiang, Fan Hua, Liu Feng-bin, Wei Chun-lin . Biological property and clinical application of tissue engineered skin [J]. Chinese Journal of Tissue Engineering Research, 2010, 14(2): 337-340. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||